Diagnosing and Treating Trigger Points
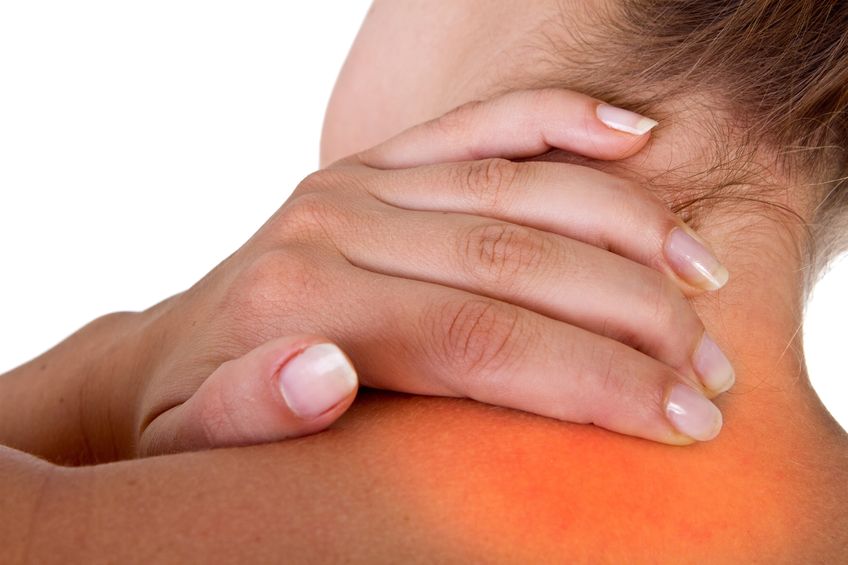
Tips for Treating Trigger Points
- To help alleviate the “knots” in the upper back and neck seek help from a Physical Therapist.
- Ask your doctor for a prescription to Physical Therapy to treat Trigger points.
- Strength training makes the muscle more resilient to the natural stress and strain that is placed on the muscle during life’s activities.
- The key to healing a Trigger Point is blood flow.
- Gently stretching the Trigger Point helps to reduce the pain that it causes. Stretching too aggressively can make the symptoms worse.
An overworked or injured muscle may form “knots” within a hypersensitive part of the muscle, causing intense pain. Known as “Trigger Points,” these “knots” are successfully treated by Physical Therapists on a daily basis. While the healthcare community does not completely agree on diagnosis or treatment, Physical Therapists and patients agree that the pain is real and the treatment is effective.
Origin of Trigger Point Research
In 1942, Dr. Janet Travell and David Simons attempted to link chronic myofacial pain to Trigger Points and developed methods to treat the nodules. As the first healthcare professionals to define Trigger Points, they suggested that the painful “point” in the muscle was related to a specific muscular injury, but not all of the time. The nodule could produce local pain, referred pain or a twitch within the muscle. These “knots” cannot be linked to specific findings of a neurological examination. Unfortunately, their diagnosis was vague.
Over the years, the medical society has not been willing to agree on a specific set of symptoms or treatment protocols for Trigger Points. Attempts to link these “knots” to myofascial pain syndromes or fibromyalgia have been minimally successful. The inability to conclusively connect Trigger Points with certain musculoskeletal conditions has fueled the fire of some who doubt of their existence.
What causes Trigger Points?
There are wide-ranging theories about the formation of a Trigger Point. One common theory states that there is a local “short circuit” of the neural signal and excess acetylcholine is released in a specific area of the muscle, causing depolarization and the contraction of several muscle cells. The injured area and prolonged, sustained muscle contraction cause a decrease in blood flow to that area.
The lack of blood flow causes a local ischemia, which begins to stimulate the nocioceptors in the muscle and produce the pain signal. Until this environment is changed and there is an increase in blood flow to the area, the pain signal continues to be transmitted. This further reduces motion and contraction force and leads to more muscle pain. With less motion, there is less blood flow through the injured area.
Another theory is similar, but deals with an injury to the Sarcoplasmic reticulm (SR) of the muscle. In this theory, the Actin and Myosin interlock during a muscle contraction, and Calcium is released by the SR to enable the interlocking to occur. When the injury occurs, the SR is unable to re-absorb the Calcium, producing a state of constant, prolonged interlocking of the muscle cells. Similar to the previously mentioned theory, this type of prolonged contraction causes a decrease in blood flow, and local ischemia which stimulates the nocioceptors and causes the pain signal to be sent to the brain.
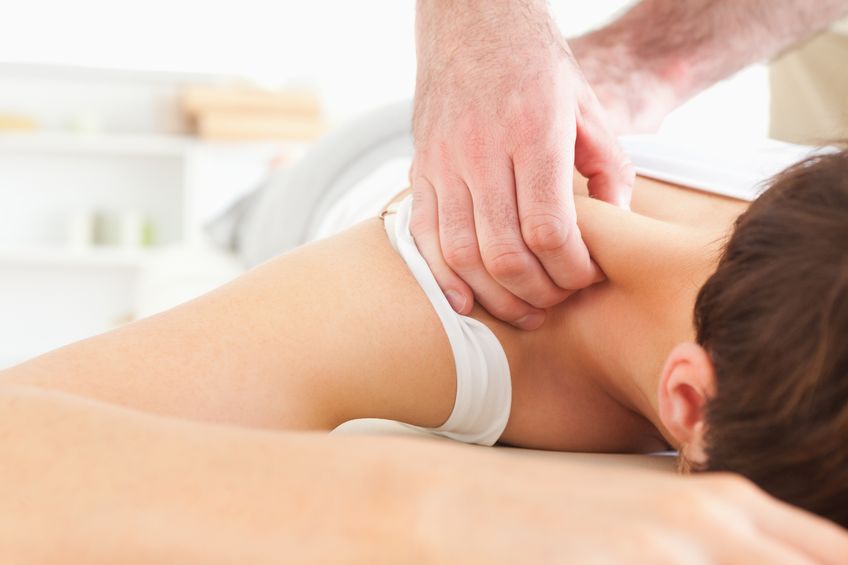
The treatments associated with Trigger Points are numerous and incorporate every aspect of Physical Therapy. In the past and present almost any type of modality such as manual therapy, injection or exercise was performed to help reduce the symptoms of a Trigger Point. Your therapist might try one of the following or a combination of several of these modalities: heat, cold, ultra sound, electric stimulation, massage, deep pressure massage, ischemic compression, vibration, spray-n-stretch, laser or dry needling. Some doctors have injected saline or cortisone into the “muscle knot.”
There are no specific protocols for treating Trigger Points. The “knot” in the patient’s muscle responds differently to various treatments and can act differently during the same treatment period. This characteristic of a Trigger Point makes it challenging to treat. Most of these treatments require a prolonged period of time to be effective.
In spite of these obstacles, Trigger Points are successfully treated by Physical Therapists on a daily basis. The treatments used are numerous and most Physical Therapists have their own bias towards specific protocols when they treat the common “knot” within a muscle. Even though the healthcare community does not agree on a common protocol, they agree that pain and resulting disability are real and should be treated.

























6/21/15
1) Can you recommend doctors in the Washington DC area who know trigger points really well?
2) Would an epidural to the nerve root ever reduce pain from trigger points?
Please reply ASAP. Thank you.
I am a bit confused on the symptoms above. I have a constant pain radian from my shoulder to the elbow that when it strike it last for a few seconds to one munite. The pain restrict me from arm mobility, the pain is felt on the back and front of the shoulder area, the chest area near the shoulder, and its severe. Any suggestion? Thank you.