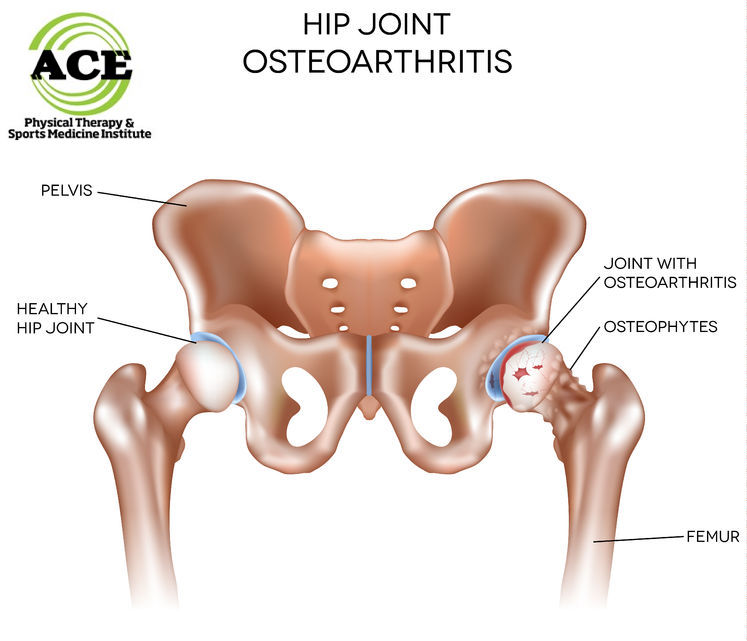
HIP OSTEOARTHRITIS AND EXERCISE

Tid Bits of Info
- The symptoms of hip OA are usually felt in the form of groin pain and stiffness.
- Some healthcare professionals profess that for every 10 lbs of body weight that is lost the pain from OA will decrease 20% or more.
- Nearly 35% of the US population will be affected by OA in their lifetime.
- OA is also referred to as Degenerative Joint Disease or DJD.
- Seek the advice and treatment of a Physical Therapist if you are diagnosed with OA.
Osteoarthritis (OA), one of the most common form of arthritic change that occurs in the body, can occur in any weight bearing joint. Hip Osteoarthritis is a common form of OA and it can lead to pain, decreased function, and an overall reduction in the quality of life. When patients suffering from Hip OA are willing to follow a prescribed exercise regimen and remain active, they normally experience less pain and can continue enjoying life activities.
OA is basically the breakdown of cartilage in the joints. The ends of bones that articulate with each other are covered with a smooth articular cartilage (hyaline cartilage). The articular cartilage is designed to withstand a tremendous amount of compressive and sheer force, but over a lifetime these forces might be too great and cause damage. When the damage occurs it cannot heal itself. The smooth surfaces become rough and rugged and these changes cause more damage as if it were a stone between two pieces of glass. Eventually, the hyaline cartilage is gone and the bone is exposed. If both sides “wear out” and the “bone-on-bone” situation occurs the symptoms of OA worsen and eventually change a person’s life.
The pain that occurs can be related to a change in the condition of the lining of the joint. The synovial lining produces fluid that is a lubricant to the joint. The roughness of the articular surfaces due to OA, leads to a proliferation and thickening of the synovial lining secondary to the increased production of fluid. This condition produces a great deal of pain because the synovial lining is inflamed. The pain leads to a reduction in neuromuscular control of the involved hip joint. The decrease in control can produce unwanted and excess motion inside the hip joint. This can cause more irritation to the articular surfaces and cause more need for the lining to produce fluid. Ultimately all of these events have a devastating impact on the joint and significantly reduce the functional capabilities of the patient.
There are many treatments for hip osteoarthritis: education, weight reduction, and exercise are the most basic. Different drugs can be prescribed to reduce the severity of the symptoms. Many studies have been conducted and have resulted in a uniform conclusion that exercising the involved hip can help to slow down the advancement of the arthritic changes and/or enhance one’s function by increasing the muscle action around the joint.
Visiting a Physical Therapist who specializes in the treatment of orthopaedic conditions can help you begin a program that will be geared towards developing muscular strength and endurance, increasing neuromuscular control and hopefully increasing the range of motion of the involved hip joint. You can visit the Physical Therapist without a doctor’s prescription for Physical Therapist but check with your insurance plan to see if you need a referral from your Primary Care Physician to visit a Physical Therapist.
Your treatment sessions with the Physical Therapist will consist of you performing exercises that are on a table and in a weight bearing position. The fact that your hip hurts should not deter you from performing exercises like squats and lunges. Obviously the Physical Therapist will modify your technique if your hip does not allow you to do the exercise with proper form. Your therapist will have your perform some form of cardiovascular exercise and core strengthening exercises. They will most likely teach stretching techniques and then they will manually stretch and mobilize your hip.
You should expect to experience some increased hip pain initially. You will be using the injured joint in ways that it has not “worked” in many years. After a few sessions the initial increase in pain will begin to get less prominent and your functional capabilities will increase. It is not unusual for it to take 6-8 weeks before you begin to “feel better.” You have to maintain your exercise routine for a life time and most of the exercises that you will be asked to perform can be performed easily in the comfort of your own home.
Hip OA is very common and can be devastating to someone’s lifestyle. The willingness to perform exercises of all kinds has been shown to be very helpful in reducing the severity of the negative symptoms associated with OA. Being active and performing specific exercises can help to impede the advancement of the arthritis and enable someone to perform the activities that are necessary or that they enjoy doing without the fear of debilitating hip pain.